
Veterans and Covid-19: What To Do?
April 30, 2020
Why Are More Men Getting Covid-19 Than Women?
June 1, 2020by Susannah Wollman
Now that parts of the country are beginning to open up after weeks of shutdown, the thought of a recurrent spike in Covid-19 cases and deaths are making people fearful. It’s important to know that the incubation period for the novel coronavirus is 2-14 days, according to the Texas Department of State Health Services.1 That means the new cases and any associated deaths are likely due to earlier contact with the virus (although technically you could be symptomatic two or three days after coming in contact). While some argue things are opening too soon, others want everything to open back up so they can go back to “life as normal.” But will life ever really be “back to normal”?
How do you know it’s safe to resume prior activities?

Testing is increasing all across America. Drive-up testing is still the safest way, at this juncture, to be tested. In an unusual show of bi-partisan agreement in Congress, House Speaker Nancy Pelosi and Sen. Majority Leader Mitch McConnell said although they were grateful for the White House’s offer of more coronavirus tests for Congress, they’d decline. “Our country’s testing capacities are continuing to scale up nationwide and Congress wants to keep directing resources to the front-line facilities where they can do the most good the most quickly,” they said in a joint statement. Congress is set to open on Monday, May 4, 2020.
If you’re ready to go back to work, this is what you should know.
- You must still follow Governor Greg Abbott’s guidelines.
- Social distancing is still in effect. That means you must maintain a separation of at least six feet from others who are not members of your household. If this restriction is not an option, you should use other methods of separation, such as covering your nose and mouth with a mask, hand hygiene, covering your cough, cleanliness and sanitation. Recent studies are showing the importance of social distancing and why we do it.
- Self-screening is necessary before entering any business. If you see any of the following symptoms, stay home
- cough
- shortness of breath
- chills
- repeated shaking with chills
- muscle pain
- headache
- sore throat
- loss of taste or smell
- diarrhea
- feeling feverish or a temperature over 100.0°
- close contact with someone who has a lab-confirmed case of Covid-19
- Wash your hands with soap and water for at least 20 seconds after entering a business or touching another person not of your household.
- Wear a face mask anytime you enter a business or are within six feet of another person.
If I had Covid-19, can I get it again?

The WHO says we just don’t have enough data to either rule it out or not. Unfortunately, some individuals are testing positive for Covid-19 after recovering and with a negative test result. Experts aren’t sure why this is happening.2
Dr. Robert Glatter,3 who is an emergency physician at Lenox Hill Hospital in New York City said in an interview, “The truth is that we don’t exactly understand the dynamics of how people who test negative after initial infection end up testing positive again. We need more studies to clarify this observed phenomenon.”
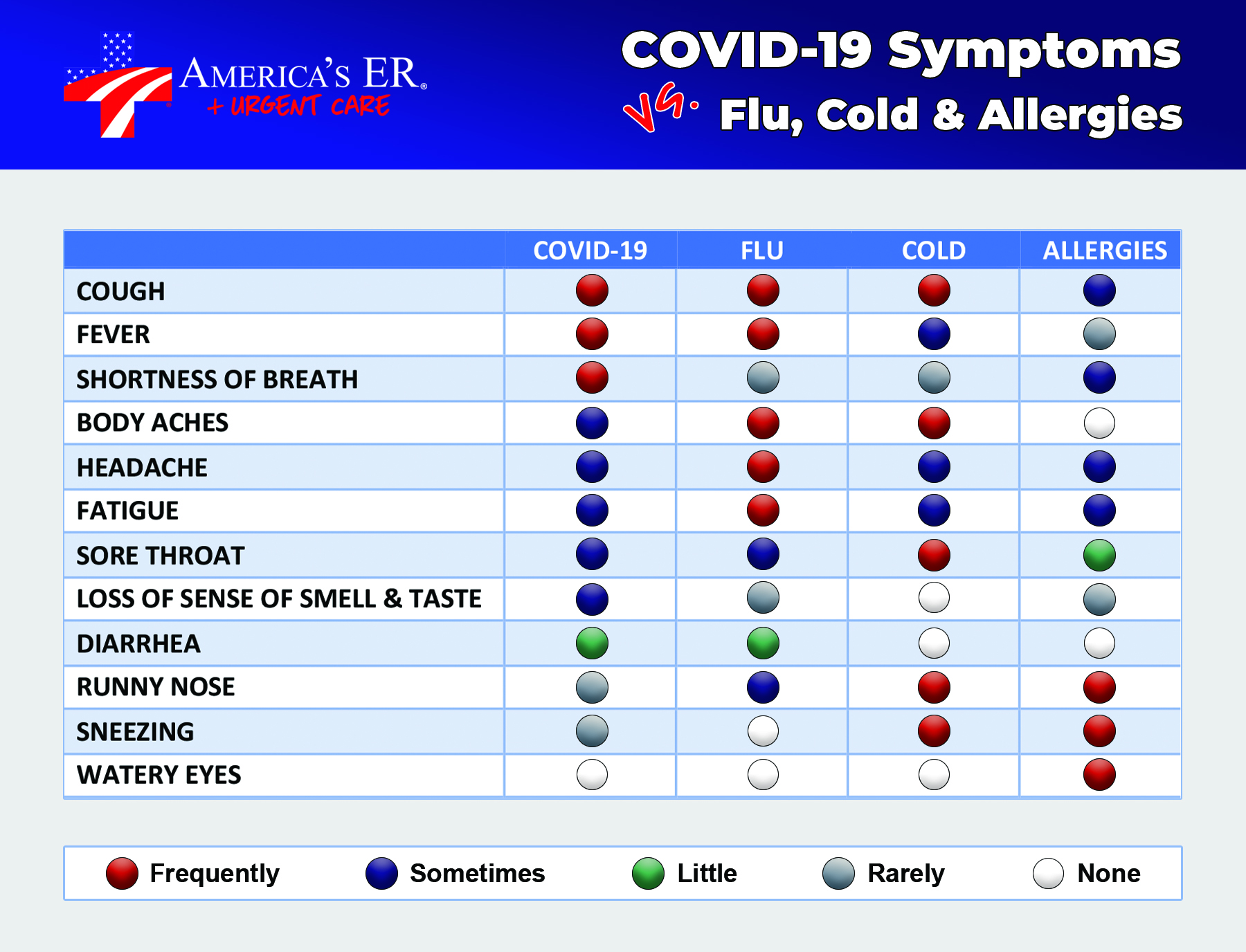
I’ve had some of the symptoms. How do I know if I’ve been infected?
One of the most frustrating characteristics of Covid-19 is that it can be asymptomatic, meaning the symptoms normally presented with the virus are simply not there, yet the person still has (or has had) the infection. All you can do is be tested. But which test? Should you get a test for the virus itself or for antibodies that your body develops as a response to the virus?
What are the differences between the test for infection and the test for antibodies?
The two tests for Covid-19 are called serology testing (antibody blood testing) and polymerase chain reaction (PCR) testing (swab test).
The PCR swab test for Covid-19 will show if you have a current viral infection. The antibody blood test can show if you’ve had the virus in the past.
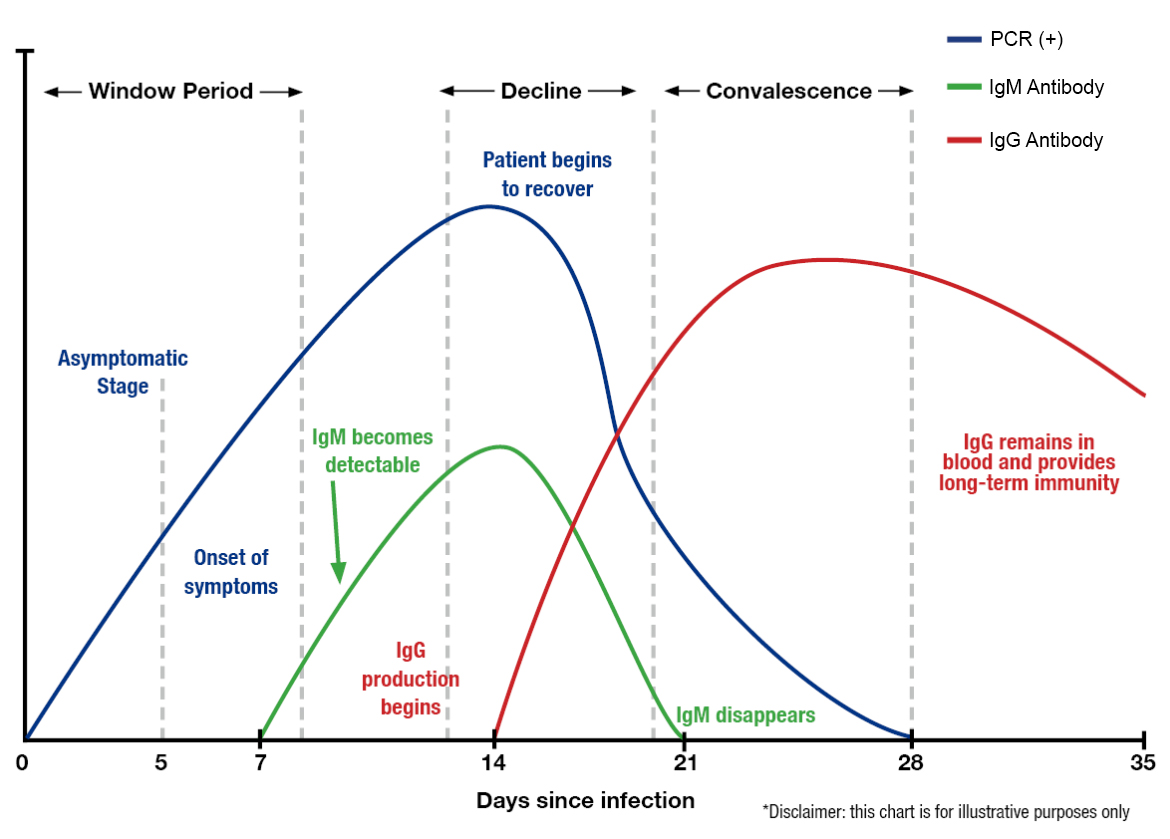
While the antibody test does not show if you currently have the coronavirus infection, it can show your body’s response to the virus and what phase of the infection you are currently in. That’s because the body takes 1-3 weeks to make antibodies once you’ve been infected. At this point in time, we don’t know if antibodies to the virus will protect you from getting the virus again. And if antibodies do protect you from re-infection, we don’t know how long that immunity might last. There just is not enough data yet to make those conclusions.
When it comes down to it, if you take one test and not the other, you are truly only seeing 50% of the full picture. You need both tests to tell you where you are on the infection curve.
America’s ER has developed a testing strategy to determine which test may be best for you.
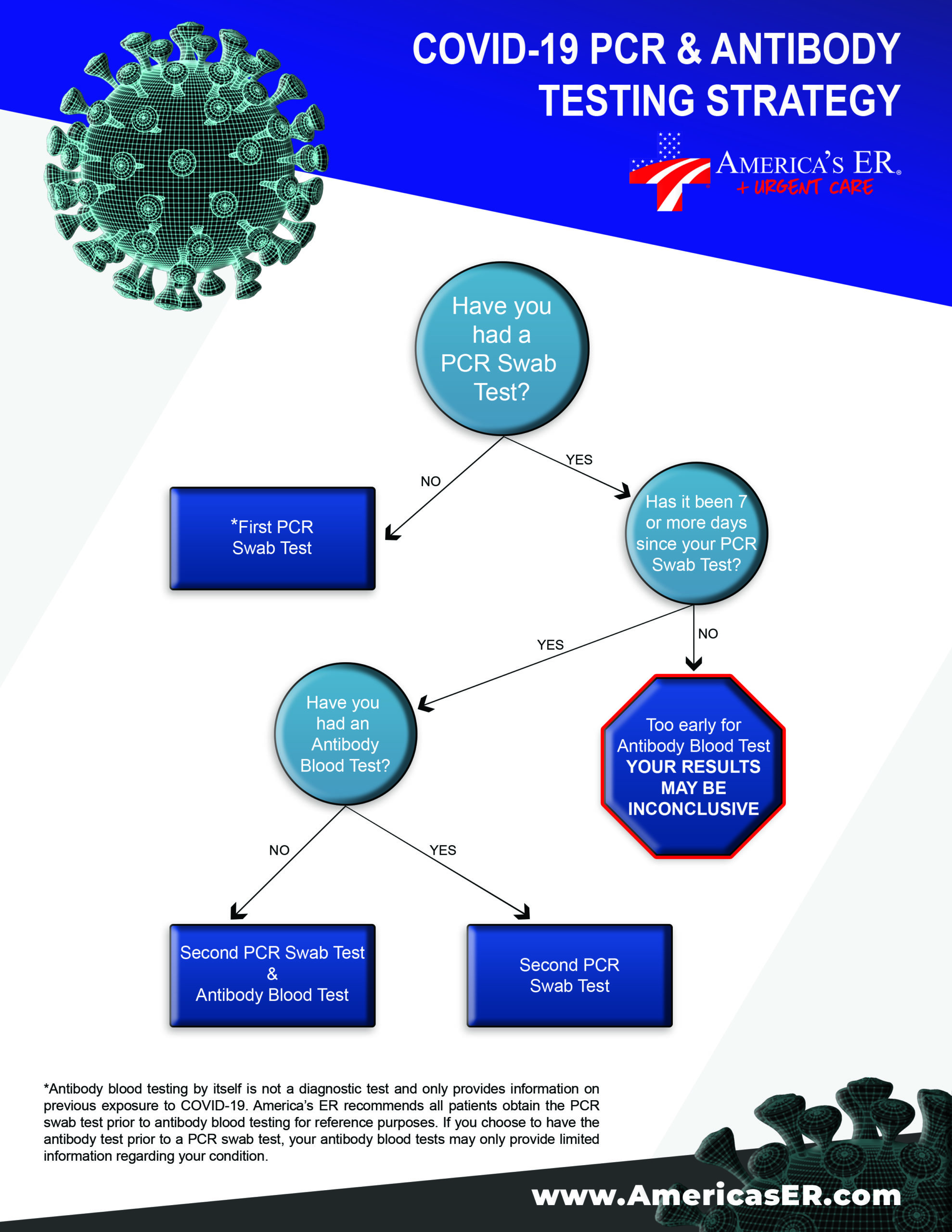

How are the tests administered?
For the PCR swab test to see if you are currently infected with COVID-19, the CDC currently approves both oral and nasal specimen collection. At America’s ER drive-through testing locations, the swab will be inserted in the back of your throat or nose and then sent to the lab for interpretation. Results typically come back in about 2-4 days.
For the antibody blood test, a small amount of blood is taken from a finger-stick (much like a glucose blood test) and then placed onto a capillary lateral flow immunoassay rapid test kit (much like a pregnancy test) which will indicate the presence of the IgM and or IgG antibody. Results are seen within 10 minutes and are provided to you while at the testing facility.
Do I need the tests?
People are getting tested for many reasons. Some are concerned they may have been exposed after learning someone they were in contact with is now showing symptoms or has a confirmed case of Covid-19. Others need proof of a negative Covid-19 test after being ill to return to work or to visit loved ones. Some people who were sick in the past are getting testing to see if the illness they had was actually COVID-19, to see if they are still shedding the virus, or to see if they may have developed antibodies to coronavirus.
The Center for Disease Control and Prevention (CDC) has guidelines for who should be tested and Governor Greg Abbott is following those recommendations. Basically, if you have symptoms of COVID-19 (or think you do) or have come in contact with someone who had a confirmed case of coronavirus, you should seek testing. If you are in Texas in one of our bigger cities (Dallas/Ft. Worth, Houston, San Antonio, or Austin, you should have no trouble finding a testing site. This map can help you find the nearest testing site to where you live.
America’s ER is currently operating a drive thru testing site (as of the date this article was published) where testing is open to anyone, regardless of symptoms. All insurance plans are accepted with zero out-of-pocket expense for both types of testing, meaning you pay nothing. The CARES Act has mandated all insurance companies are required to cover all costs associated with COVID-19 testing by law. If you insurance company refuses to pay for your testing, they are breaking the law. For those without insurance, America’s ER offers a self-pay options for both PCR and antibody testing. Learn more about it here.
What do I do if I test positive?
If you test positive for Covid-19, there are certain protocols you should follow.
- If you only have mild symptoms, stay at home and take care of yourself as you would for the flu or a cold. Follow CDC guidelines.
- If your symptoms get worse, call your doctor.
- If you are over 65, especially if you have underlying health conditions, call your doctor immediately.
- If you are caring for someone else, you can find more information on the Texas Health Trace website.
If I test negative, am I out of the woods?
No one is out of the woods until the coronavirus is completely contained or eradicated. You can return to work and resume normal activities if you take precautions. The CDC recommends but does not require people to wear face masks when going out in public. There are many online resources for making simple, cloth face masks.
Cloth face masks actually may not protect you from getting the virus. But it may prevent someone else from getting Covid-19 because as mentioned (above), you may have the virus and not even know it. Face masks can help us all prevent the spread of Covid-19.
Footnotes
[1] Texas Department of State Health Services. “Coronavirus Disease 2019 (COVID-19).”
[2] Ries, Julia. “Can You Develop COVID-19 Twice? Here’s What We Know.” Healthline, Healthline Media, 27 Apr. 2020.
[3] March 21st, 2020, et al. “Robert Glatter, MD.” Robert Glatter, MD | Northwell Health.




